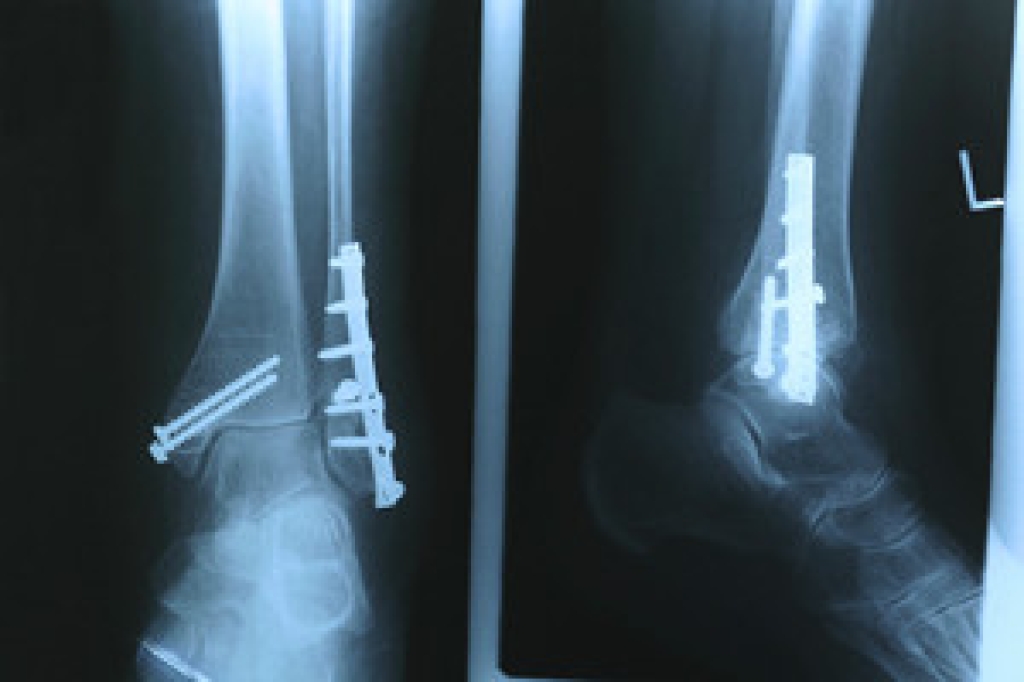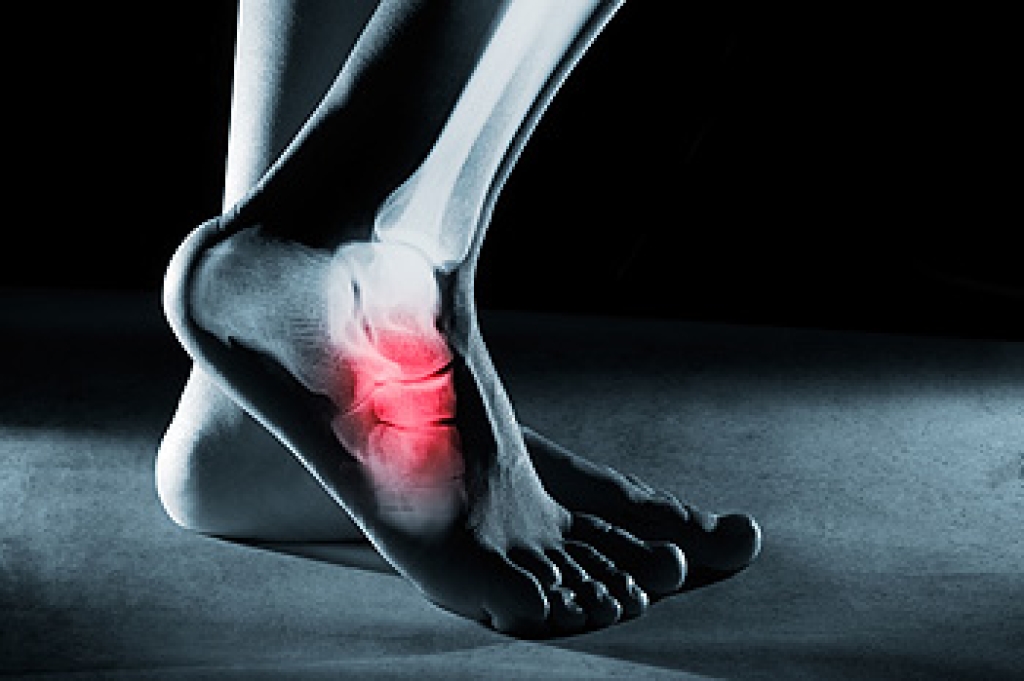
A foot stress fracture manifests as a small crack or severe bruising within a bone, typically caused by repetitive force or overuse, such as high-impact activities like running or jumping. This injury often results from sudden increases in activity intensity or duration, wearing inadequate footwear support, or changes in training surfaces. Symptoms can include localized pain and tenderness, swelling, and difficulty bearing weight on the affected foot. The pain associated with a stress fracture is often described as dull and achy initially, worsening with activity and subsiding with rest. In some cases, there may be a noticeable tenderness or throbbing sensation at the fracture site. Prompt diagnosis through imaging techniques like X-rays or MRI scans is essential to differentiate a stress fracture from other foot injuries and initiate appropriate treatment. If you have foot pain, and believe it may be a stress fracture, it is suggested that you visit a podiatrist who can determine what the most appropriate course of treatment is for you.
Activities where too much pressure is put on the feet can cause stress fractures. To learn more, contact one of our podiatrists from Footcare Now. Our doctors can provide the care you need to keep your pain free and on your feet.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures occur in the foot and ankle when muscles in these areas weaken from too much or too little use. The feet and ankles then lose support when walking or running from the impact of the ground. Since there is no protection, the bones receive the full impact of each step. Stress on the feet can cause cracks to form in the bones, thus creating stress fractures.
What Are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
- Runners
- People affected with Osteoporosis
- Tennis or basketball players
- Gymnasts
- High impact workouts
Symptoms
Pain from the fractures occur in the area of the fractures and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity which involves high impact will aggravate pain.
If you have any questions please contact our offices located in Elmhurst Jackson Heights, Astoria, Rego Park, and Forest Hills, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.